The Scottish Health Survey 2008
The Scottish Health Survey 2008
7 OBESITY
Linsay Gray and Alastair Leyland
SUMMARY
- In 2008 the majority of adults aged 16 or over (68.5% of men and 61.8% of women) were either overweight ( BMI of 25 to less than 30 kg/m 2) or obese ( BMI of 30 kg/m 2 and over). Overall obesity prevalence in 2008 was 26.0% for men and 27.5% for women.
- There has been a steady upward trend in the prevalence of overweight and obesity among both sexes aged 16 to 64 since 1995. 55.6% of men aged 16-64 were overweight or obese in 1995 compared with 66.3% in 2008. The equivalent increase for women was from 47.2% to 59.6%.
- 15.9% of men aged 16 to 64 were obese in 1995 compared with 24.9% in 2008. The equivalent figures for women were 17.3% and 26.5%. The proportion who were morbidly obese tripled between 1995 and 2003, from 0.5% to 1.8% in men and from 1.3% to 3.6% in women. The equivalent rates for 2008 were 1.4% and 3.5%, respectively, which suggest that morbid obesity prevalence has stabilised.
- Mean BMI has also increased over time from 26.0 kg/ m 2 in 1995 to 27.2 kg/ m 2 in 2008 among men, and from 25.7 kg/ m 2 in 1995 to 27.3 kg/ m 2 in 2008 among women.
- The majority of children aged 2 to 15 (61.8% of boys and 71.3% of girls) had a BMI classified as healthy. Similar proportions of boys and girls were underweight (2.1% of boys and 1.9% of girls). Boys were more likely than girls to have a BMI outwith the healthy range (38.2% versus 28.7%), and were also more likely to be overweight, including obese (36.1% versus 26.9%).
- The proportion of boys with a BMI outwith the healthy range increased from 29.2% in 1998, to 33.9% in 2003, to 38.2% in 2008. In contrast, the corresponding figures for girls have remained very similar with no significant change over the years (30.4%, 30.7% and 28.7%, respectively).
- The age-standardised prevalence of obesity did not vary greatly between men according to their socio-economic classification, but it did for women. 24.0% of women in managerial and professional households were obese, this rose significantly to 34.7% and 28.5% among those in lower supervisory and technical, and semi-routine and routine households, respectively. Patterns in the age-standardised prevalence of overweight including obesity were less obvious in relation to socio-economic classification.
- Patterns in the age-standardised prevalence of obesity across equivalised household income quintiles appeared to differ for men and women: whereas obesity prevalence was lowest among men in the lowest income quintile, for women those in the highest quintile were the least likely to be obese. The patterns for overweight including obesity were broadly similar.
- Men and women in the most deprived areas had the highest age-standardised prevalence of obesity. For men, in contrast with obesity, being overweight or obese had clear reverse gradients with area deprivation. Men in the least deprived areas were more likely to be overweight or obese than men in the most deprived areas. For women, the corresponding patterns were broadly in line with those for obesity.
- Regression analysis was used to explore the relationship between a range of factors and the odds of being overweight (including obese), and being obese. The odds of being overweight or obese increased with age, and were higher for people with medium or low physical activity levels. Current smokers had lower odds than people who had never smoked. Being overweight or obese was also associated with equivalised household income but in opposite ways for men and women. Men in small employer and own account worker households, and those in semi-routine and routine households, had significantly higher odds of being overweight or obese compared with those in managerial and professional households. Men who were cohabiting, single, divorced or widowed had lower odds of being overweight or obese compared with married men. Women living in the 1st (most), 2nd and 3rd deprived area quintiles had significantly increased odds of being overweight or obese.
- The findings for obesity were similar to those for overweight, with associations with age, marital status, cigarette smoking status, and physical activity for both men and women, and additionally with equivalised household income and area deprivation for women only.
7.1 INTRODUCTION
The first Scottish Health Survey in 1995 found that the majority of men were overweight or obese, the same was true of women by 1998. 1 These figures have worsened over time; the proportion of adults who were obese increased by 46% between 1995 and 2003. The obesity problem is widespread in many parts of the world. The World Health Organisation has described the situation as an epidemic and its most recent estimate suggests that 1.6 billion adults worldwide are overweight, of whom at least 400 million are obese. 2 However, Scotland has one of the worst obesity records amongst developed countries with levels that are higher than those in most other European countries. 3 Based on current trends the UK Government Office for Science's Foresight Report on obesity forecasts that by 2050 as many as 50% of women and 60% of men in England could be obese. 4 The outlook for Scotland is unlikely to be any better.
These obesity trends are an increasing cause of ill-health in Scotland and a contributing factor in many deaths. The Scottish Public Health Observatory estimates that 47% of type 2 diabetes can be attributed to obesity, 36% of hypertension, 18% of myocardial infarction, 15% of angina and 12% of osteoarthritis, 5 indicating the wide range of conditions for which causal links with obesity has been suggested. Obesity has also been shown to be associated with, but not necessarily a direct cause of, respiratory conditions, sleep disturbance, infertility and mental ill-health. 4, 6 Obesity not only has a major impact on people's quality of life, it also increases the risk of hospitalisation 5 and early death. 7, 8
The wider social and economic costs of obesity are significant. In 2003 it was estimated that the cost to the NHS in Scotland of obesity and obesity-related illnesses was in the region of £171 million. 9 Forecasts based on the NHS budget in England suggest that the proportion of NHS expenditure attributable to increasing overweight and obesity could double between 2007 and 2050. 4
Tackling obesity is a key priority for the public health sector in Scotland. Of the many factors associated with the development of obesity, physical inactivity (see Chapter 6 in this report) and poor diet (see Chapter 5) are often seen as the biggest causes and the two factors for which the evidence is most robust. 5, 10 Although increasing activity and improving diet may appear straightforward, there is growing recognition that the ways in which wider societal influences shape people's opportunities to exercise and exert choices over their diet mean that strategies to prevent weight gain need to look beyond solutions targeted at individuals. 4 Many of the initiatives focusing on exercise and diet that have been launched in recent years have the potential to impact on obesity levels, including initiatives and targets relating to diet described in Chapter 5 and those for physical activity described in Chapter 6. However, the Scottish Government's Healthy Eating, Active Living: An action plan to improve diet, increase physical activity and tackle obesity (2008-2011), published in 2008, is the first to draw these factors together into a single Government approach and make obesity a central focus. 11 In addition, this document contains a commitment to use the Foresight Report 4 on obesity as the basis for its new longer-term obesity strategy for Scotland. Specific actions to help obese individuals are also part of the Keep Well initiative that is attempting to address health inequalities via interventions targeted at deprived communities. 12
In addition to the measures being taken to address obesity among adults one of the Scottish Government's National Performance Framework national indicators, 13 as set out in Chapter 1 of this Report, focuses on child healthy weight and is being monitored via the Scottish Health Survey: 14
Reduce the rate of increase in the proportion of children with their Body Mass Index outwith a healthy weight.
Although this Report's main focus is on adult health, the headline data for this important indicator for children are presented in this chapter. More detailed analysis of children's weight will be published in 2010. Healthy Eating, Active Living11 outlines a number of steps being taken in Scotland to help promote child healthy weight. These include a programme of healthy weight interventions aimed at 20,000 children, which is supported by an NHS Scotland HEAT15 target to meet the agreed rates of completion for these interventions by 2010/11.
This chapter focuses on body mass index ( BMI), derived from the direct measurements of height and weight taken in the main interview. Although BMI is not a perfect measure of body fat (see discussion below) accurate height and weight measurements are relatively easy to obtain in population surveys. This approach is certainly preferable to self-reported measures of height and weight which are known to be subject to considerable misreporting. 16 Other measures of obesity can be derived from waist and hip measurements, which have been included in the last three Scottish Health Survey reports. Waist and hip measurements are predictors of some health conditions, independent of BMI, and are considered by some to be preferable to BMI. 17 Waist and hip measurements are taken during the nurse visit in which, from 2008, only a sub-sample of the participants are invited to participate. For this reason the analysis of obesity based on waist and hip measurements will be published in 2010 when two years of nurse data have accumulated.
This chapter first outlines the methods of the height and weight measurements and the derivation of BMI. This is followed by an examination of age-sex distributions of height and weight for adults, and BMI for both adults and children (as noted above). Trends over time in adult BMI between 1995, 1998, 2003 and 2008, and between 1998, 2003 and 2008 for children, are then presented. The relationships between adult obesity prevalence and three key socio-demographic variables ( NS-SEC, equivalised household income, and the Scottish Index of Multiple Deprivation) are also examined. This is followed by regression analysis to look at the relationship between adult BMI and various risk factors (including physical activity, alcohol consumption, fruit and vegetable intake, and socio-demographic characteristics).
7.2 METHODS AND DEFINITIONS OF MEASUREMENT
Full details of the protocols for carrying out the measurements are contained in Volume 2 of this report and are briefly summarised here.
7.2.1 Height
Height was measured using a portable stadiometer with a sliding head plate, a base plate and three connecting rods marked with a metric measuring scale. Participants were asked to remove shoes. One measurement was taken, with the participant stretching to the maximum height and the head positioned in the Frankfort plane. 18 The reading was recorded to the nearest millimetre.
7.2.2 Weight
Weight was measured using Soehnle and Tanita electronic scales with a digital display. Participants were asked to remove shoes and any bulky clothing. A single measurement was recorded to the nearest 100g. Participants aged under 2 years, or who were pregnant, or chairbound, or unsteady on their feet were not weighed. Participants who weighed more than 130 kg were asked for their estimated weights because the scales are inaccurate above this level. These estimated weights were included in the analysis.
In the analysis of height and weight, data from those who were considered by the interviewer to have unreliable measurements, for example those who had excessive clothing on, were excluded from the analysis.
7.2.3 Body Mass Index ( BMI)
The Body Mass Index ( BMI), defined as weight (kg)/height (m2), is a widely accepted measure that allows for differences in weight due to height. It has been used in each Scottish Health Survey report to date. However, BMI has some limitations. 17, 19 It does not distinguish between mass due to body fat and mass due to muscular physique. It also does not take account of the distribution of fat.
BMI was calculated for all those participants for whom a valid height and weight measurement was recorded. Adult participants were classified into the following BMI groups: 20
| BMI (kg/m 2) |
Description |
|---|---|
| Less than 18.5 |
Underweight |
| 18.5 to less than 25 |
Normal |
| 25 to less than 30 |
Overweight |
| 30 to less than 40 |
Obese, excluding morbidly obese |
| 40+ |
Morbidly obese |
Other cut off points are also used in analyses of obesity, for example the WHO cites evidence that chronic disease is an increasing risk in populations when BMI exceeds 21, 2 while mortality rates do not necessarily correlate neatly with the categories presented here. 8 However, meaningful comparisons of prevalence estimates between countries require agreed thresholds and these categories correspond with the WHO's recommended definitions for underweight, normal, overweight and obese (though they use three sub-classifications of obesity rather than the two presented here). 21 In the first two SHeS reports the normal weight range for BMI was taken as over 20 to 25 kg/m 2, but medical opinion now regards it as more appropriate to define it as 18.5 to less than 25 kg/m 2, and this report, in common with the report of the 2003 survey, continues to use this revised definition. The tables of age and sex prevalence report mean BMI and the five categories outlined above. Although obesity has the greatest ill-health and mortality consequences overweight is also a major public health concern, not least because overweight people are at high risk of becoming obese, while underweight also has negative health consequences. The trend and socio-demographic tables present three measures: the proportion who are either overweight or obese ( BMI of 25 kg/m 2 or more), the proportion who are obese ( BMI of 30 kg/m 2 or more), and the proportion morbidly obese ( BMI of 40 kg/m 2 or more). The latter group are at particularly high risk of morbidity and mortality. 22
Despite the relatively wide acceptance of the use of BMI as an adiposity indicator, the establishment of a specific obesity and overweight classification system for young people has proved to be difficult. Constant changes in body composition during growth mean that the relationship between weight-for-height and adiposity during childhood and adolescence is age-dependent, and this relationship is further complicated by ethnicity and gender. 23 Several methods have been employed to define early life overweight and obesity, including body fatness as measured by skinfold thickness, 24, 25 national BMI percentile charts, 26, 27, 28 weight-for-height indices, 29BMI percentile cut-off points, 30 and international 31 and national 32BMI cut-off points.
Percentile charts can be used to compare an individual child's BMI with the distribution of BMI in a reference population to see whether it corresponds with the average or whether it is unusually high or low. Since children's BMI changes as they age, the comparison needs to be age specific. For example the BMI for a child of 5 needs to be compared with a reference population with a large enough sample of 5 year olds rather than data for children with a wide age range.
The classifications of children's BMI used in this chapter, set out below, have been derived from BMI percentiles of the UK reference curves 27, 28 (referred to as the National BMI percentiles classification); these were also used in the 2003 and 1998 Scottish Health Surveys.
| Percentile cut-off |
Description |
|---|---|
| At or below 5 th percentile |
Underweight |
| Above 5 th percentile and below 85 th percentile |
Healthy weight |
| At or above 85 th percentile and below 95 th percentile |
Overweight |
| At or above 95 th percentile and below 98 th percentile |
Obese |
| At or above 98 th percentile |
Morbidly obese |
The 85 th / 95 th cut-off points are commonly accepted thresholds used to analyse overweight and obesity in children. These thresholds have previously been used to describe childhood overweight and obesity prevalence trends in the UK. 33, 34, 35, 36 The National BMI percentiles classification has been shown to be reasonably sensitive (i.e. not classifying obese children as non-obese) and specific (i.e. not classifying non-obese children as obese). 37, 38 As noted in the introduction, one of the Scottish Government's National Indicators relates to healthy weight in children, defined as neither underweight nor overweight / obese. For this reason the data have been categorised to show the total proportions that are overweight, obese or morbidly obese, as well as the proportion underweight.
The use of reference curves require children's ages to be exactly matched to those in the reference population charts. This is a fairly straightforward process in clinical settings where an individual child's exact age can be compared with the look-up chart for their age. With survey data it is not as easy to calculate an exact age for every child within the sample. To overcome this, in 1998 and 2003 children's ages were rounded to the nearest half year (e.g. 2, 2.5, 3) and the corresponding reference points for the rounded ages were used. From 2008 onwards a different method of calculating children's ages is being used that plots the exact ages of the children in the sample without needing to round their ages in this way. 39 The same method has been applied to the 1998 and 2003 data so the trend table presents updated measures of children's BMI for those years.
Although children's exact age was used to calculate the BMI grouping prevalence rates (based on the interview date and the date of birth), the results are presented using grouped ages based on age at last birthday.
7.3 RESPONSE TO ANTHROPOMETRIC MEASUREMENTS, BY AGE AND SEX
Response to anthropometric measurements among adults is shown in Table 7.1. A valid height measurement was obtained for 89% of men and women. Among men this decreased from 94% at age 16-24 to 80% at age 75 and over; the equivalent figures for women were 92% and 76%, respectively. 87% of men and 86% of women provided a valid weight measurement and, with known height could, therefore, have their BMI derived. As with height, the proportions providing valid weight measurements declined with age with the lowest levels in those aged 75 and over. A valid BMI was derived for 85% of boys and girls, response was generally higher among children aged 4 and over (data not shown). Children whose BMI was more than three standard deviations from the average for their age were excluded from the analysis. Table 7.1
7.4 HEIGHT AND WEIGHT, BY AGE AND SEX
7.4.1 Height
With mean height of 175.0 cm, men were almost 14 cm taller than women (mean height 161.3 cm) on average, as shown in Table 7.2. Mean height varied significantly across the age groups, peaking at 178.2 cm in men aged 25-34 and at 163.8 cm in women aged 16-24, and declining steadily over age to 168.4 cm in men and 154.8 cm in women aged 75 and over. Table 7.2
7.4.2 Weight
On average, men (mean weight of 83.9 kg) were just under 13 kg heavier than women (mean weight 71.3 kg), shown in Table 7.3. There were significant differences in weight over age: in men, weight initially rose with increasing age to a peak that ranged between 87.5 kg and 86.6 between the ages of 35 to 64. It fell slightly to 85.9 kg in those aged 65-74, with a bigger drop thereafter to 78.4 kg in the oldest age group. In women, the peak weight (74.4 kg) occurred later than for men, in those aged 55-64, decreasing to 66.3 kg in the oldest group. Table 7.3
7.5 ADULT BMI
7.5.1 BMI by age and sex
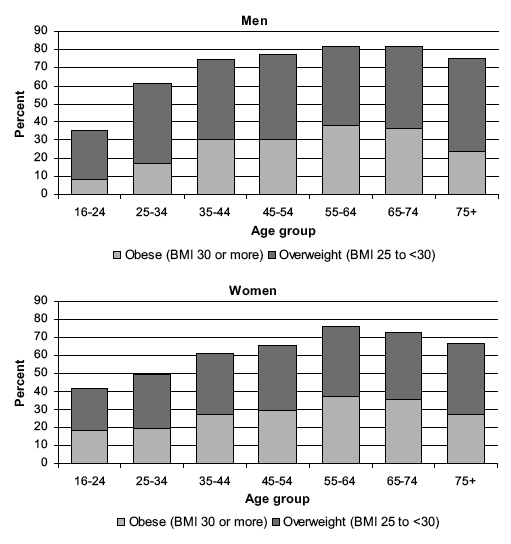
Table 7.4 presents the prevalence figures for the five BMI classifications discussed above (from underweight to morbidly obese) as well as summary measures of overweight including obese ( BMI 25 kg/m 2 or more) and obese ( BMI 30 kg/m 2 or more) by age and sex in 2008. Figure 7A below presents the figures for overweight and obese. Overall obesity prevalence in adults aged 16 and over in 2008 was 26.0% for men and 27.5% for women. There were significant differences in the distribution of BMI by age: among men, obesity prevalence was lowest at 8.0% among those aged 16-24, rising to 38.1% in those aged 55-64, falling to 23.5% in the oldest group. Among women, the youngest group had higher prevalence of obesity (18.3%) than their male counterparts; this rose to 36.9% in those aged 55-64, falling to 27.1% for the oldest age group. Overweight, including obese prevalence was 68.5% for men and 61.8% for women and followed similar patterns by age to obesity. Underweight prevalence was 2.0% for men and 1.9% for women and was most common among the youngest age groups, falling with increasing age to middle-age and rising slightly for the older groups. Although more men than women aged 16-24 were underweight (8.2% versus 4.7%) the sample sizes for this age group are small so the difference must not be over-interpreted. Table 7.4, Figure 7A
Figure 7A Prevalence of overweight and obese, by sex
7.5.2 Trends in adult BMI
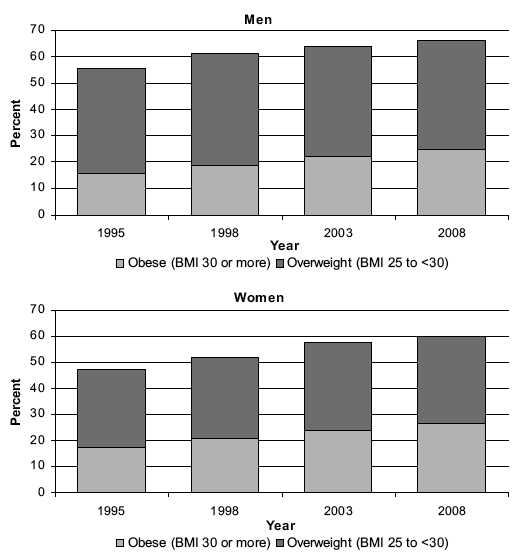
Table 7.5 and Figure 7B show the prevalence of obesity ( BMI 30 kg/m 2 or more), and overweight, including obese ( BMI 25 kg/m 2 or more) by age in the previous survey years - 1995, 1998, 2003 - and the current survey year, 2008. Changes to the sample composition in the four survey years mean that the figures for adults presented here are based only on those aged 16 to 64. The steady rise in obesity prevalence seen over the last decade or so has continued to 2008. Among men aged 16 to 64, the prevalence of obesity has risen from 15.9% in 1995, to 18.8% in 1998, 22.0% in 2003 and now to 24.9% in 2008. The equivalent figures for women are 17.3%, 20.9%, 23.8%, and now 26.5%. Overweight including obese has also shown corresponding increases in both sexes, rising steadily from 55.6% in 1995 to 66.3% in 2008 among men, and from 47.2% in 1995 to 59.6% in 2008 among women. Morbid obesity ( BMI of 40 kg/m 2 or more) prevalence has risen from 0.5% in 1995 to 1.8% in 2003 and 1.4% in 2008 among men and from 1.3% in 1995 to 3.6% in 2003 and 3.5% in 2008 among women. These changes between 2003 and 2008 are not significant and suggest that the prevalence of morbid obesity may have stabilised. Mean BMI among those aged 16 to 64 has also increased over time from 26.0 kg/m 2 in 1995, now standing at 27.2 kg/m 2 in 2008 among men and from 25.7 kg/m 2 in 1995, now standing at 27.3 kg/m 2 in 2008 among women. Table 7.5, Figure 7B
Figure 7B Prevalence of overweight and obese (aged 16 to 64), 1995, 1998, 2003, 2008, by age and sex
7.6 CHILDREN'S BMI
7.6.1 BMI by age and sex
Table 7.6 shows the proportions of children aged 2-15 who were underweight, healthy weight, overweight, obese and morbidly obese in 2008. The majority of children - 61.8% of boys and 71.3% of girls - had a BMI classified as healthy. Similar proportions of boys and girls were underweight (2.1% of boys and 1.9% of girls). Boys were more likely than girls to have a BMI outwith the healthy range (38.2% versus 28.7%), and were also more likely to be overweight, including obese (36.1% versus 26.9%). Table 7.6
7.6.2 Trends in children's BMI
Table 7.7 reports the percentages of children aged 2-15 classified as having a BMI outwith the healthy range, and the prevalence of overweight, including obese, in 1998, 2003 and 2008. As noted above, the method for calculating children's ages for use with the UK reference charts has changed so the data for 1998 and 2003 presented in Table 7.7 differ slightly to that presented in previous reports. The proportion of boys with a BMI outwith the healthy range increased across the three survey years, from 29.2% in 1998, to 33.9% in 2003, to 38.2% in 2008. In contrast, the corresponding figures for girls have remained very similar with no significant change over the years (30.4%, 30.7% and 28.7%, respectively). The increase in the proportion of boys outwith the healthy weight range is accounted for by a corresponding increase in the proportion who were overweight or obese, rather than significant changes in the prevalence of underweight. 27.8% of boys aged 2-15 were overweight in 1998, compared with 32.4% in 2003 and 36.1% in 2008. There were no significant changes among girls aged 2-15 in this period. The Health Survey for England has found similar trends in that the prevalence of overweight or obesity increased significantly among boys in the 2000-2007 period (from 27% to 31%), but not among girls. 40 However, the sample size for children in 2008 is smaller than it has been in previous survey years so more detailed analysis of this change over time, and comparisons with England, will need to be carried out by aggregating the 2008 and 2009 data. Table 7.7
7.7 OVERWEIGHT AND OBESITY, BY SOCIO-DEMOGRAPHIC FACTORS
Tables 7.8 to 7.10 present mean BMI and the prevalence of overweight, obesity and morbid obesity for adults by socio-economic classification ( NS-SEC of the household reference person), equivalised household income and the Scottish Index of Multiple Deprivation (descriptions of each of these measures are available in the Glossary at the end of this volume). To ensure that the comparisons presented in this section are not confounded by the different age profiles of the sub-groups, the data have been age-standardised (for a description of age-standardisation please refer to the Glossary). On the whole the differences between observed and age-standardised percentages are small. Therefore, the percentages and means presented in the text below are standardised. The tables report both the observed and the age-standardised figures.
7.7.1 Socio-economic classification ( NS-SEC)
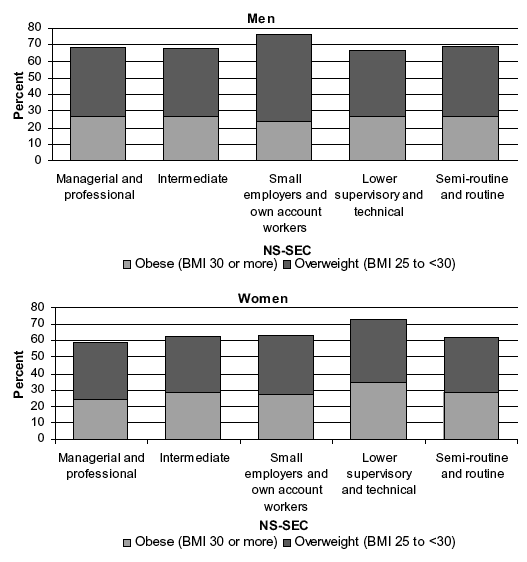
The age-standardised prevalence of obesity among men and women by NS-SEC of the household reference person is given in Table 7.7 and Figure 7C. Obesity prevalence did not vary greatly by household NS-SEC among men, although those in small employer and own account worker households had the lowest level at 23.9%. There were clearer patterns among women, with the lowest age-standardised prevalence being 24.0% among those in managerial and professional households, rising significantly to 34.7% among those in lower supervisory and technical households. Overweight including obese was relatively constant across NS-SEC groups for men, although those in small employer and own account worker households had the highest prevalence (76.5%). Variations in overweight (including obese) prevalence across NS-SEC in women followed a similar pattern to that for obesity; the lowest level was found among those in managerial and professional households (58.7%) and was highest among those in lower supervisory and technical households (72.8%). Morbid obesity in men varied, but not systematically, by NS-SEC ranging from 0.8% in the intermediate group to 2.4% in lower supervisory and technical households. Patterns were more obvious among women, with an age-standardised prevalence of 2.0% in managerial and professional households and 4.6% in semi-routine and routine households. Mean BMI was around 27 kg/m 2 - 28 kg/m 2 for all NS-SEC groups among men; there was greater fluctuation among women with significant rises from 26.8 kg/m 2 in managerial and professional households, to 28.7 kg/m 2 in lower supervisory and technical households. Table 7.8, Figure 7C
Figure 7C Prevalence of overweight and obese (age-standardised), by NS-SEC of household reference person and sex
7.7.2 Equivalised household income
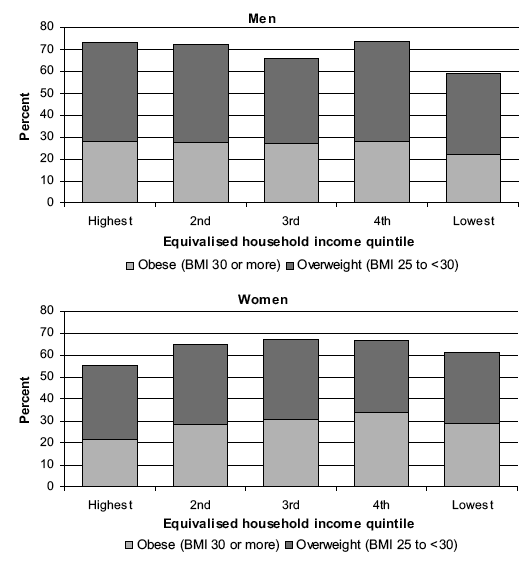
Table 7.8 and Figure 7D show obesity prevalence by quintiles of equivalised household income for men and women. Patterns in obesity across equivalised household income quintiles appeared to differ for men and women: whereas obesity prevalence was lowest among men in the lowest income quintile, for women those in the highest quintile were the least likely to be obese. To illustrate, the age-standardised prevalence of obesity was 21.7% among men in the lowest income quintile and ranged between 26.8% and 28.1% in the four other groups. Among women, the age-standardised prevalence of obesity was 21.6% in the highest income quintile and ranged between 28.5% and 34.0% in the four other quintiles. The patterns for overweight including obesity by equivalised household income were broadly similar to those for obesity; men in the lowest income households and women in the highest income households were the least likely to be overweight or obese. Gradients in morbid obesity were more consistent for both sexes, with the lowest prevalence found in the highest and second income quintiles, and the highest prevalence in the 4 th and lowest income quintiles. The differences between the income groups were more pronounced among women, and were statistically significant; just 1.1% of women in the highest income quintile were morbidly obese compared with 5.0% and 4.3% of those in the fourth and fifth lowest quintiles, respectively. Mean BMI tended to follow the same patterns as with overweight and obesity prevalence, with men in the lowest income quintile, and women in the highest, having the lowest age-standardised mean BMI. These differences between the income groups were significant for both sexes. Table 7.9, Figure 7D
Figure 7D Prevalence of overweight and obese (age-standardised), by equivalised household income quintile and sex
7.7.3 Scottish Index of Multiple Deprivation ( SIMD)
Two measures of SIMD are being used throughout this report. The first, which uses quintiles, enables comparisons to be drawn between the most and least deprived 20% of areas and the three intermediate quintiles, and helps to assess the extent of any inequalities in behaviours or outcomes. The second contrasts the most deprived 15% of areas with the rest of Scotland (described in the tables as the "85% least deprived areas"). The most deprived 15% of areas have been identified as of particular concern by Scottish Government and are the subject of a number of policy initiatives. The Scottish Health Survey is designed to provide a large enough sample in the SIMD 15% areas after four years to enable robust detailed analysis at this level.
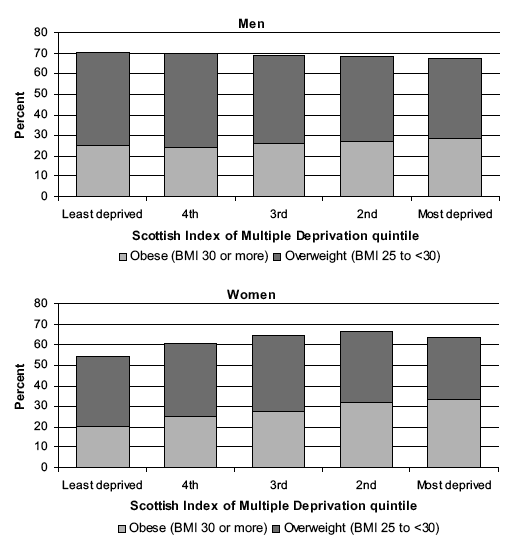
Of the socio-demographic factors considered, women's obesity was most clearly patterned by area deprivation (Table 7.9 and Figure 7E). Obesity prevalence among men did not differ significantly across the quintiles. For women, the prevalence rose steadily and significantly with increasing area deprivation from 20.1% in the 5 th (least) deprived to 33.3% in the 1 st (most) deprived. Overweight, including obese was not significantly associated with SIMD among men. For women, the patterns in overweight, including obese were broadly in line with those for obesity, with the lowest level of 54.3% in the 5 th (least) deprived quintile, rising to between 63.7% and 66.5% in the three most deprived quintiles. Mean BMI was stable across SIMD quintile groups for men but rose with increasing deprivation among women.
The differences between the results for the 15% most deprived areas and the rest of Scotland for the age-standardised prevalence of overweight including obese and obesity, and mean BMI were generally small and not statistically significant. The one exception was obesity among women, for whom 32.3% of those living in the 15% most deprived areas compared with 26.7% of those living in the rest of Scotland were obese. Table 7.10, Figure 7E
Figure 7E Prevalence of overweight and obese (age-standardised), by Scottish Index of Multiple Deprivation quintile and sex
7.8 FACTORS ASSOCIATED WITH OVERWEIGHT AND OBESITY
7.8.1 Overweight including obese
Logistic regression was used to investigate the socio-demographic and behavioural factors associated with overweight, including obese ( BMI 25 kg/m 2 or more) separately for men and women. In these analyses, the odds of a reference category (shown in the table with a value of 1) is compared with that of the other categories for individual factors. In this example, an odds ratio of greater than 1 indicates that the group in question has higher odds of being overweight or obese than the chosen reference category, and an odds ratio of less than 1 means they have lower odds. By simultaneously controlling for a number of factors, the independent effect each factor has on the variable of interest can be established. For more information about logistic regression models and how to interpret their results see the glossary at the end of this volume.
The odds ratios for overweight including obese are presented in Table 7.11. The factors found to be significantly associated with being overweight or obese were: age, equivalised household income quintile, cigarette smoking and physical activity; additionally, NS-SEC and marital status were significant for men and SIMD quintile for women. The results for these are reported below. Parental NS-SEC, fruit and vegetable consumption and alcohol intake were also included in the analysis but were not found to be significant.
Age was associated with being overweight or obese. All men aged 25 and over and all women aged 35 and over had significantly higher odds of being overweight or obese than the youngest group with odds ratios largest in men (odds ratio 3.92) and women aged 55-64 (odds ratio of 3.70).
Being overweight or obese was independently associated with equivalised household income but in opposite ways for men and women. The odds of being overweight or obese were significantly lower among men in the 3 rd and 5 th (lowest) income quintiles compared with those of men in the highest quintile (odds ratios of 0.64 and 0.48 respectively). For women, the odds were significantly higher among those in the 4 th income quintile compared with those in the highest quintile (odds ratio of 1.63).
Cigarette smoking status was associated with being overweight or obese. Current smokers had significantly lower odds of being overweight or obese compared with those who never smoked (odds ratios of 0.60 for men and 0.73 for women).
Physical activity levels were associated with being overweight or obese. Three levels of physical activity were analysed: high (30 minutes or more at least 5 days a week); medium (30 minutes or more on 1 to 4 days a week); and low (fewer than 30 minutes of activity a week). The high level of activity category was used as the reference group. Compared with those in the high physical activity group, those with medium and low levels of physical activity had significantly increased odds of being overweight or obese (odds ratios of 1.76 in men and women for the medium activity group and 1.73 in men and 2.00 in women for the low activity group).
For men only, household NS-SEC was associated with being overweight or obese. Those living in small employer and own account worker households and those in semi-routine and routine households had significantly higher odds of being overweight or obese compared with those in managerial and professional households (odds ratios of 2.12 and 1.48 respectively). Marital/partnership status was also associated with being overweight or obese in men, with living as married, single, divorced and widowed men having significantly lower odds of being overweight or obese compared with married men (odds ratios of 0.52, 0.44, 0.59 and 0.57 respectively).
Among women, being overweight or obese was associated with SIMD quintile. Women living in the 1 st (most) deprived, 2 nd and 3 rd quintiles had significantly increased odds of being overweight or obese (odds ratios of 1.40, 1.54 and 1.37 respectively). Table 7.11
7.8.2 Obesity
Logistic regression was also used to examine the factors associated with obesity ( BMI 30 kg/m 2 or more) separately for men and women. The odds ratios for obesity are given in Table 7.12. Age, marital status, cigarette smoking status and physical activity were significantly associated with the odds of being obese in both men and women. Additionally, equivalised household income and SIMD quintile were associated with obesity in women.
Compared with those aged 16-24, the odds of being obese were significantly elevated across almost all age groups for both men and women; the exceptions were those over 75, and women aged 25-34.
Marital/partnership status was associated with obesity, with significantly decreased odds seen in men who were living as married or single (odds ratios of 0.60 and 0.55, respectively) compared with married men. The pattern was different for women: divorced women had significantly lower odds of being obese compared with married women (odds ratio of 0.63).
Current smoking was associated with significantly decreased odds of being obese compared with people who had never smoked for both men (odds ratio of 0.48) and women (odds ratio of 0.73).
Compared with those attaining high physical activity levels, those with medium and low levels had significantly higher odds of being obese (odds ratios of 1.82 in men and 1.72 in women with medium levels; 2.32 in men and 2.76 in women with low levels).
Among women, living in households in the 4 th income quintiles was significantly associated with an increased odds of being obese compared with those in the highest income quintile (odds ratios of 1.57).
Women living in the three most deprived area quintiles were at significantly higher odds of being obese compared with those in the least deprived quintile (odds ratios of 1.42 for the 3 rd quintile, 1.77 for the 2 nd quintile and 1.82 for the 1 st (most) deprived quintile). Table 7.12
There is a problem
Thanks for your feedback