Better Cancer Care, An Action Plan
Better Cancer Care, An Action Plan outlines the way forward for cancer services, which are required to support all those in Scotland who find themselves living with and beyond cancer.
SECTION FIVE: REFERRAL AND DIAGNOSIS
The key components of successful cancer management include:
- Recognising and reporting symptoms early
- Expertise in identifying patients who require prompt referral
- Rapid access to investigations and treatment.
This is underpinned by good inter-professional communication, a highly-trained workforce and excellent two-way communication between healthcare workers and patients/carers.
Recognising Symptoms
The cancer journey for many people starts when they notice symptoms. For others, however, even though survival rates and patient outcomes are improving and cancer is now very often a long-term condition, many people are reluctant to present, even when they have symptoms.
Evidence gathered from audits in primary care, as a result of nationally devised and locally-driven enhanced services for cancer care, indicates that patients frequently have symptoms for a considerable period of time before reporting them and seeking help (Figure 11). Findings from this audit must be acted upon to encourage people to see their GPs earlier to enable faster referral into diagnostic and treatment services. In order to achieve this, more work needs to be done with patients and their representatives to explore and further understand the issues that make them reluctant to come forward.
"A lot of men and women are terrified of going to a doctor to find out if they have cancer." Better Cancer Care Conference Workshop Participant |
Figure 11: Time from patients noticing and reporting symptoms to GPs and time from patients reporting symptoms to GP referral to secondary care
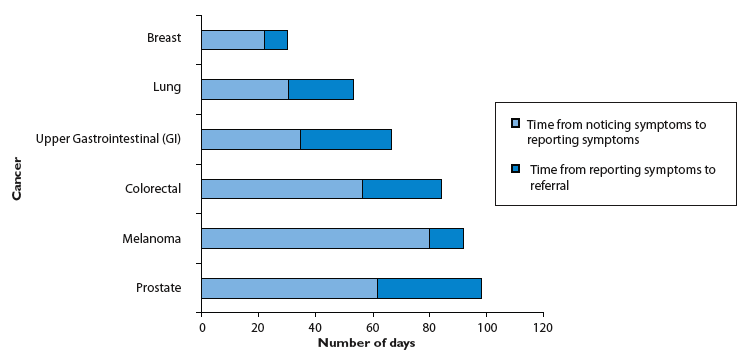
Source: Scottish Primary Care Cancer Group
Referral Process
HDL (2007) 09 Scottish Referral Guidelines for Suspected Cancer assists GPs and others to make an informed decision on their patients' conditions. While some people who are subsequently found to have cancer present with specific symptoms, such as a persistent lump, blood in sputum or a definite change in bowel habit, others present with much vaguer symptoms. It is important to remember that GPs will see many patients with signs and symptoms which, though similar, will turn out to be due to other common, benign ailments.
Timely referral from primary to secondary care is extremely important and best practice suggests that all such referrals should be submitted electronically. Electronic referral reduces the time taken for a referral to be received and acted upon. Some systems now depend entirely on electronic referral, but data from the 2005/2006 primary care-based cancer referral audit reported levels of electronic referral that varied from 14% to 51% of all urgent referrals. Whilst the use of electronic referral has improved significantly, scope for further improvement remains. Cancer networks and NHS Boards must consider how best to improve electronic referral rates, establishing systems in secondary and tertiary care services to triage all referrals (whether received electronically or by other means) in a more timely manner.
The use of specific cancer-related protocols was examined as part of the above audit and showed that a pro forma was used in only 24% of urgent referrals. While it is likely that this may also have improved over time, cancer networks and NHS Boards must consider the best use of appropriate templates to speed up the whole referral process.
Examples of Good Practice in Scotland
Redesign of Referral and Investigations Pathways Reducing Unnecessary Delays in:
Lung Cancer
GPs can directly refer patients for a chest x-ray. In some NHS Boards where the radiologist reporting the x-ray suspects a diagnosis of lung cancer, a direct referral to the chest clinic to be seen by a respiratory physician or for a CT scan can be arranged with simultaneous notification to the patient's GP. This ensures rapid access to further investigations, diagnosis and treatment, thereby reducing waiting times.
Colorectal Cancer
In some NHS Boards, referrals for patients with symptoms suspicious of bowel cancer are triaged on receipt and if appropriate, patients are sent direct to test (colonoscopy or flexible sigmoidoscopy and barium enema). This reduces the number of clinic appointments a patient needs to attend and speeds the pathway to diagnosis.
Investigations
Where appropriate, and in keeping with best evidence guidelines, initial investigations should be conducted in primary care prior to referral unless a suspected diagnosis of cancer is evident. Where specialised investigations are required these should be offered in a timely way, that are sensitive to the patient's needs and provided as locally as possible.
Work undertaken by the Scottish Government Diagnostics Collaborative Programme has improved the availability of specialist investigations including those for suspected cancer. No patient should wait longer than nine weeks for CT, Magnetic Resonance Imaging ( MRI), Ultrasound, Barium Enema, Upper and Lower Endoscopy and Cystoscopy, and this will inevitably benefit those eventually diagnosed with cancer.
All NHS Boards have effectively achieved the nine-week waiting times target for radiology and endoscopy services ahead of the target date of December 2007. This was due to the successful implementation of a variety of high-impact changes and improvements at local level, for example:
- NHS Forth Valley reduced the wait for CT scans from 12 weeks to six weeks by introducing extended day working
- NHS Lanarkshire introduced straight-to-test models, cutting unnecessary hospital visits and improving waiting times for outpatients and endoscopy
- NHS Greater Glasgow & Clyde introduced patient-focused booking for radiology and endoscopy services reducing patient Did Not Attend ( DNA) rates to less than 5% and improving patient satisfaction.
As part of the 18 weeks referral to treatment programme, it is expected that any waiting times for these key tests will be minimised. As part of this strategy, NHS Boards are working towards a maximum wait of six weeks from March 2009.
Positron Emission Tomography
A relatively new diagnostic tool in cancer investigations is Positron Emission Tomography ( PET), allied to CT ( PET/ CT). This is a form of scanning that depends on cancer cell function rather than solely assessing its size. It detects cancer cells that may not be picked up by other imaging technologies. After treatment such as chemotherapy, it may indicate whether a lump is simply scar tissue or active cancer.
After the announcement of an initial £5 million investment in 2004, the Scottish PET Advisory Group was formed to oversee the introduction of this service. Modern PET/ CT scanners are now operational in Aberdeen and Glasgow. Edinburgh has the use of a mobile scanner, pending the completion of installation works for a permanent machine expected to be clinically operational in 2009. In 2008, the Scottish Government approved the business case for the installation of a PET/ CT facility in Dundee.
PET is being developed as a Scotland-wide service with a single point of entry for appointments, to ensure that any patient needing a scan will receive it as soon as possible at whichever centre has the first available appointment. The clinical indications for PET scanning have grown rapidly in recent years. Clinical protocols based on best evidence for specific tumour types have been developed and are reviewed regularly by expert groups in Scotland.
All of these PET/ CT facilities are being developed in close collaboration with relevant universities and medical schools. These facilities will greatly strengthen Scotland's ability to take forward ambitious research proposals nationally and internationally and will eventually be accompanied by a cyclotron to generate the isotopes (radioactive material) necessary for research as well as routine clinical use. A Scottish PET Research Group was established to ensure maximal advantage is taken of the opportunities currently available and to coordinate efforts with the PET Research Group of the UK's National Cancer Research Institute, which has published a PET Research Strategy.
We will:
- Work with the Scottish Primary Care Cancer Group, NHS Health Scotland, health promotion teams, voluntary groups, patients and others to assess how to improve public awareness of common cancer symptoms to encourage patients to present early
- Work with partners (including regional cancer networks, NHS Boards and the Scottish Primary Care Cancer Group) to audit levels of electronic referral and support NHS Boards to further increase such referrals in line with established best practice
- Improve the process of electronic referrals so that all such referrals include GP practice email addresses
- Establish live links between all local electronic systems and agreed local referral guidelines based on HDL (2007) 09 Scottish Referral Guidelines for Suspected Cancer
- Work with NHS Boards to explore the potential for the redesign of referral and investigations pathways, to reduce unnecessary delays
- Identify a designated primary care lead with responsibility for cancer within each NHS Board, with a remit that includes contributing to the development and evaluation of cancer services across the whole patient pathway and in particular, at the boundaries between primary and secondary care
- Continue nationally devised and locally driven enhanced services for cancer care in primary care. These should support improvements in direct cancer care and in cancer services development
- Continue to work to develop a collaborative which will organise Scotland-wide PET services
- Take advantage of future PET/ CT research opportunities in Scotland and elsewhere.
There is a problem
Thanks for your feedback